Evidence based practice
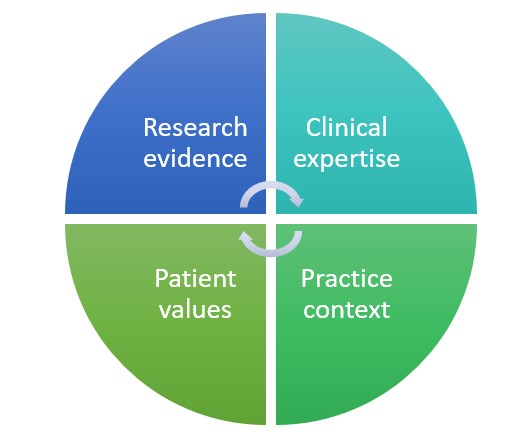
Evidence based medicine was first defined by Sackett et al. as “the conscientious, explicit, and judicious use of current best evidence in making decisions about the care of individual patients” (1996, p. 71). Evidence based medicine has since expanded to evidence based practice to apply more widely to other health professions (e.g. physiotherapy, social work, nursing etc.) and other disciplines (e.g. education and librarianship). It is the integration of best available research evidence, clinical expertise, and patient values and preferences. More recent models incorporate a fourth component, the clinical practice context (Hoffman et al., 2017).
The steps in EBP
There are five essential steps in EBP:
- Ask: Convert the patient problem into an answerable question
- Acquire: Find the best evidence to answer the question
- Appraise: Critically appraise the validity and applicability of the evidence
- Apply: Integrate the appraised evidence in the clinical setting
- Act: Evaluate the performance and success of the change
This module focuses on the first three steps in the cycle: developing an answerable question, finding the best evidence to answer the question, and appraising the quality of the evidence.